The country is three and a half months into the rollout of emergency use COVID-19 vaccines, a process that we hope will end massive lockdowns and help get schools reopened. While the CDC provided suggested guidelines for prioritizing vaccines, each state was allowed to create their own plan for the process. As data becomes available, we’ve watched it to see what we can learn about the decisions being made.
Let’s start by reviewing the determination for phased rollouts of the vaccine. The CDC went through a lengthy process to create a set of guidelines for who should first receive the vaccines. Their process included a look at the data, the impact on communities, and an ethical review of the decisions. Some have asked me why the elderly were prioritized in the early phases. The comments of some indicated that since these citizens were older and had less years of life ahead of them, then they should be at the back of the line.
If young people were dying or being hospitalized in great numbers from COVID, that might be a strategy to consider. But they aren’t. While most age groups have similar chances of contracting COVID, the CDC tells us that those over 65 have a significant increase in hospitalizations and deaths.
Data: CDC; Table: Joy Eakins
In fact, in Kansas, citizens over the age of 65 accounted for 78% of all hospitalizations and 92% of all deaths reported due to COVID. That strain on ICUs, healthcare workers, and communities are diminished more quickly by vaccinating these high-risk individuals first.
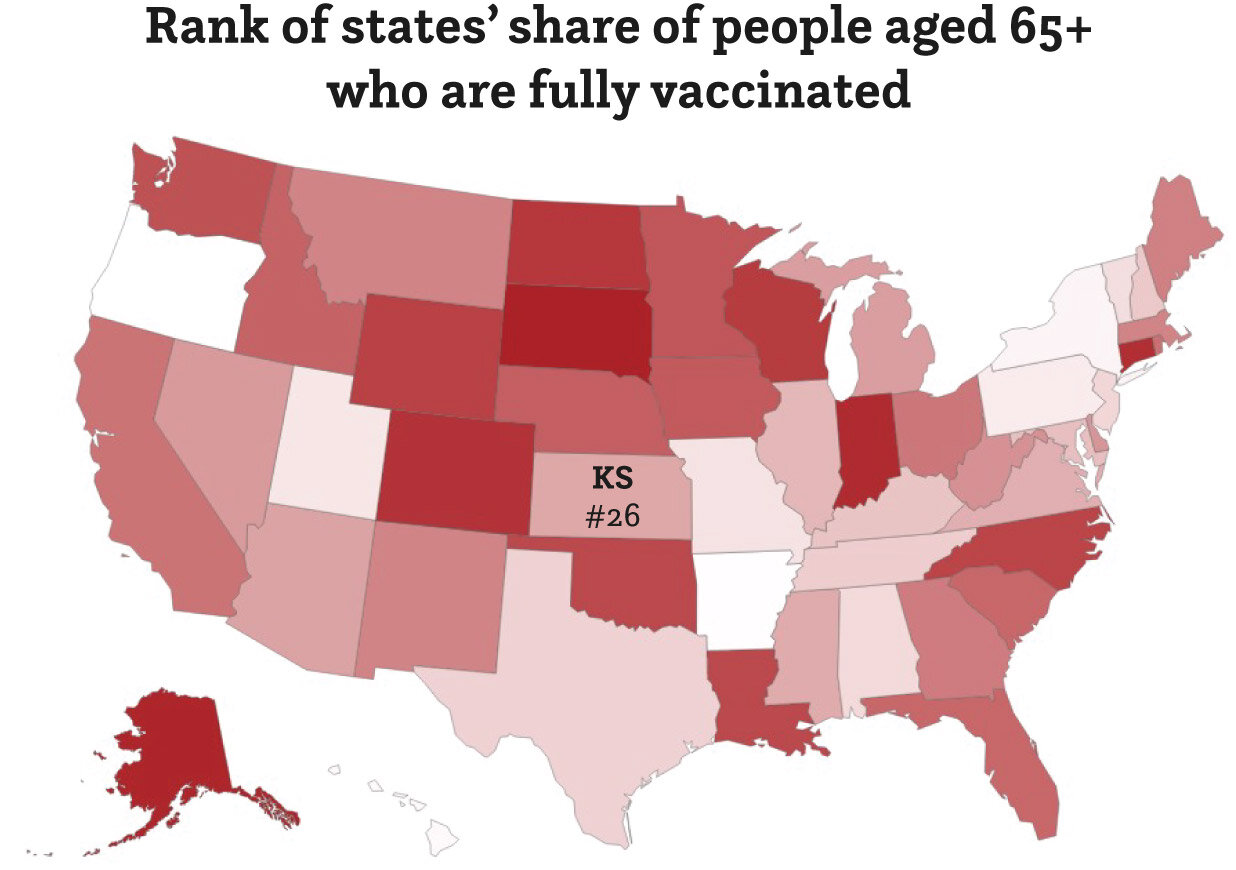
Many states did follow CDC guidelines on that initial phase for healthcare workers and Long Term Care facility residents and staff. But after those initial stages, there are differences in practice resulting in different results as demonstrated in the map below.
Data: CDC; Map: Joy Eakins
This map shows the percent of those 65+ who have been vaccinated in each state. Oregon senior citizens waited the longest to be eligible for their vaccines -most waiting behind teachers who received priority. The hope was that prioritizing teachers would open schools earlier. However, Oregon 6th to 12th graders remain in remote learning even today.
South Dakota ranks first in that same measure, with over 60% of their seniors being fully vaccinated. One reason South Dakota believes they are successful in the rollout is that their medical systems have created a process that allows citizens to fill out online forms now indicating which priority group they belong to. This gives the healthcare teams an understanding of the demand and allows them to proactively release vaccine to each phase. And, as each phase becomes available, they can proactively contact their citizens and get them scheduled. (Becker)
As of March 29, Kansas ranks 32nd with an average of just over 42% of our seniors being fully vaccinated. In many counties, seniors have struggled to find open appointments when they became eligible or had to endure long lines in the cold (ABC). Many without nearby family found it difficult to navigate the process or saw their appointments cancelled when supplies ran short. Senior independent living facilities were not included in the federal immunization plan either, leaving many who thought they would be covered wondering how to find their immunization. (AP)
Another metric used in reviewing effectiveness of the rollout is the number of doses administered versus the number distributed to the state.This percentage allows us to see whether states are effectively rolling out the vaccine after they receive it.
Data: CDC; Map: Joy Eakins
In Kansas, there has been plenty of controversy and criticism of the rollout and the fact that we have regularly ranked near the bottom for percent administered. In early January, the CDC’s data showed that Kansas had the lowest rate in the country for vaccine distribution, and as of March 29, we have risen to a rank of 38, even though we rank 17th in the number of doses delivered per 100,000 residents. In discussions about the rollout, officials have blamed issues with the reporting system and delays in getting the data. When pressed, officials have blamed a lack of data-gathering and said that Kansas had prioritized getting vaccines into people’s arms over tracking the data real-time.
Unfortunately, this response further demonstrates the lack of understanding by our leaders about how data can inform policy decisions and processes. Good data processes would model the population of each county and be able to predict how much each county needed based on the phase being targeted in the state. Each county could understand the number of vaccines they were expected to provide per day and staff accordingly based on the number being delivered. As those numbers changed, the feedback would be added to the model and new communications could be automated for counties to review. But beyond that modeling, a good feedback system would help alert the state when counties were falling behind their targeted administration numbers.
Had this process been in place in Kansas, it could have headed off a significant issue with our own administration. Large counties in Kansas were predominantly given the Pfizer vaccine because of its storage requirements. But as Pfizer fell behind in its expected allotments and Moderna sped up its deliveries, the state did not adjust its allotments. Accordingly, some urban counties received as much as one-third of the expected doses per 100 residents as other rural counties. This increased wait times in Sedgwick County as well as Shawnee, Wyandotte and Johnson. Today those counties still have the lowest rates of vaccination in the state. In the meantime, the State has had to resort to a manual reporting process from every vaccine administrator to understand what has been received and distributed by county because of the widespread data issues with their WebIZ system. (Topeka) In our initial review of the spreadsheet, we found multiple sources reporting administration rates over 100%, indicating that this spreadsheet is also unreliable. (KDHE Vaccine)
Kanas has certainly stumbled out of the gate with the vaccine rollout, leaving us all at risk. But there is still time to improve our outcomes if we will make the investment to understand the importance of our own data and commit to the process.